Outpatient physician services in Switzerland have historically been reimbursed using the TARMED fee-for-service tariff, introduced in 2004 and largely unchanged for more than two decades [1]. In response to structural limitations and growing pressure for reform, the Swiss Federal Council approved a new outpatient tariff system consisting of the TARDOC individual service tariff in combination with outpatient flat rates, which together replaced TARMED as of 1 January 2026 [2,3].
This reform represents a substantial change in how ambulatory services are documented, coded, and reimbursed, with implications for clinical workflows and departmental resource allocation [4]. While economic and administrative aspects of the transition have been widely discussed, little attention has been paid to how well surgical residents—who increasingly face operational and leadership responsibilities—understand billing systems or perceive their relevance.
International literature suggests that billing education is inconsistently integrated into postgraduate training and that residents frequently report inadequate knowledge despite recognizing its importance [5–7]. Therefore, we conducted an exploratory survey to describe surgical residents’ familiarity with billing systems, perceived barriers to engagement, and educational needs in the early phase of TARDOC implementation.
Methods
Study design and participants
This was a cross-sectional, anonymous survey targeting surgical residents working in Switzerland. Participation was voluntary and uncompensated. The survey was conducted between 30 November 2025 and 11 January 2026.
Survey dissemination
The questionnaire was distributed via LinkedIn, targeted dissemination within hospitals affiliated with Swiss/Knife, and the Swiss Young Surgeons newsletter.
Survey content
The survey assessed:
- training stage and hospital type,
- familiarity with billing systems,
- direct exposure to billing processes,
- sources of information on billing and TARDOC,
- perceived barriers to engagement,
- perceived importance of billing knowledge,
- prior training and educational preferences,
- work priorities and perceived indirect effects of billing,
- and open-ended qualitative feedback.
Multiple responses were allowed where appropriate.
Data analysis
Data were analyzed descriptively and are reported as absolute numbers and percentages. Given the small sample size and exploratory design, no inferential statistical analyses were performed.
Results
Participant characteristics
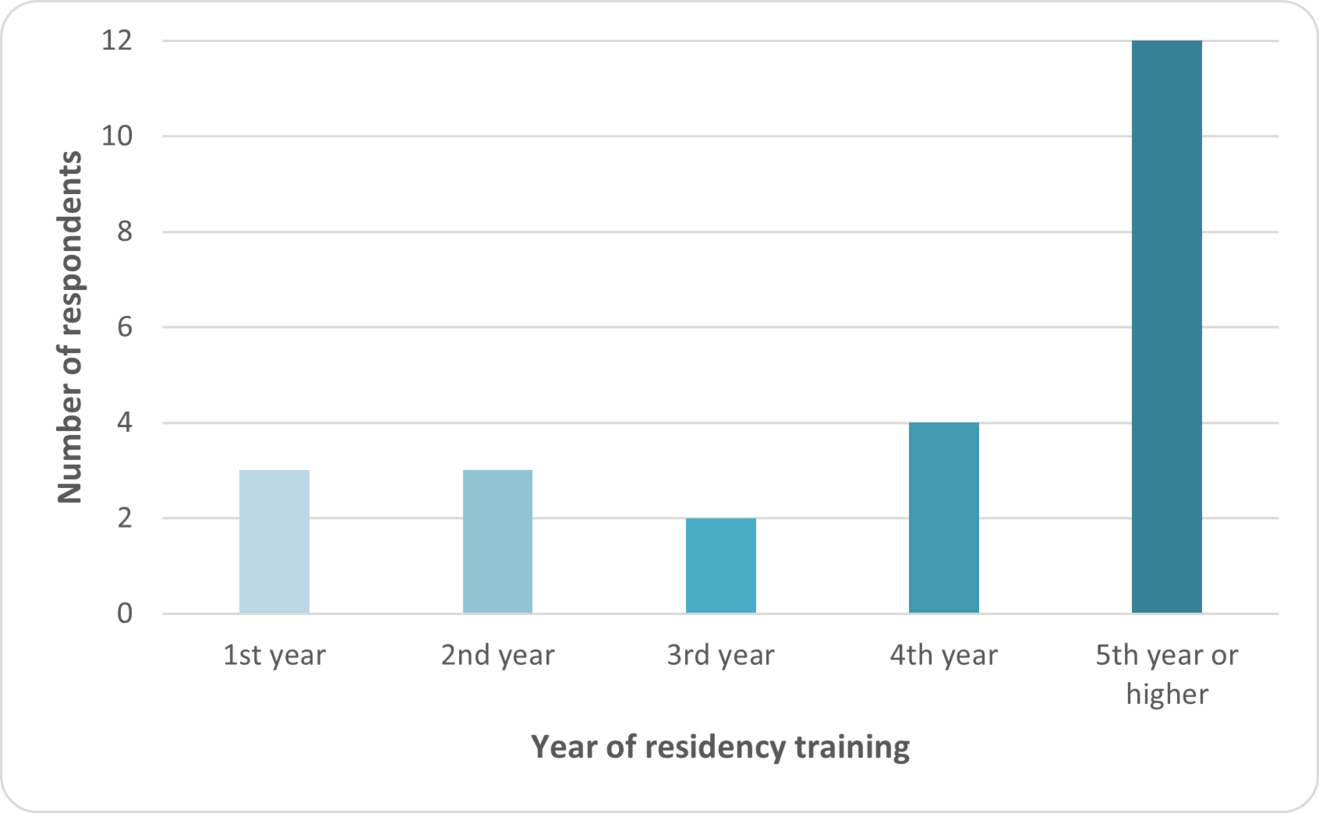
A total of 24 residents participated in the questionnaire. Half of respondents were in their fifth year of residency or beyond (12/24, 50%), indicating a predominance of senior trainees.
Most participants worked in university (11/24, 46%) or cantonal hospitals (7/24, 29%), with fewer from regional hospitals (5/24, 21%) and private clinics (1/24, 4%).
Taken together, the cohort primarily reflects perspectives from senior residents in large public institutions.
Familiarity with billing systems and exposure
Self-reported familiarity with billing systems was low. Only 6/24 (25%) reported moderate familiarity, while 18/24 (75%) reported little or no familiarity; no participant reported good familiarity.
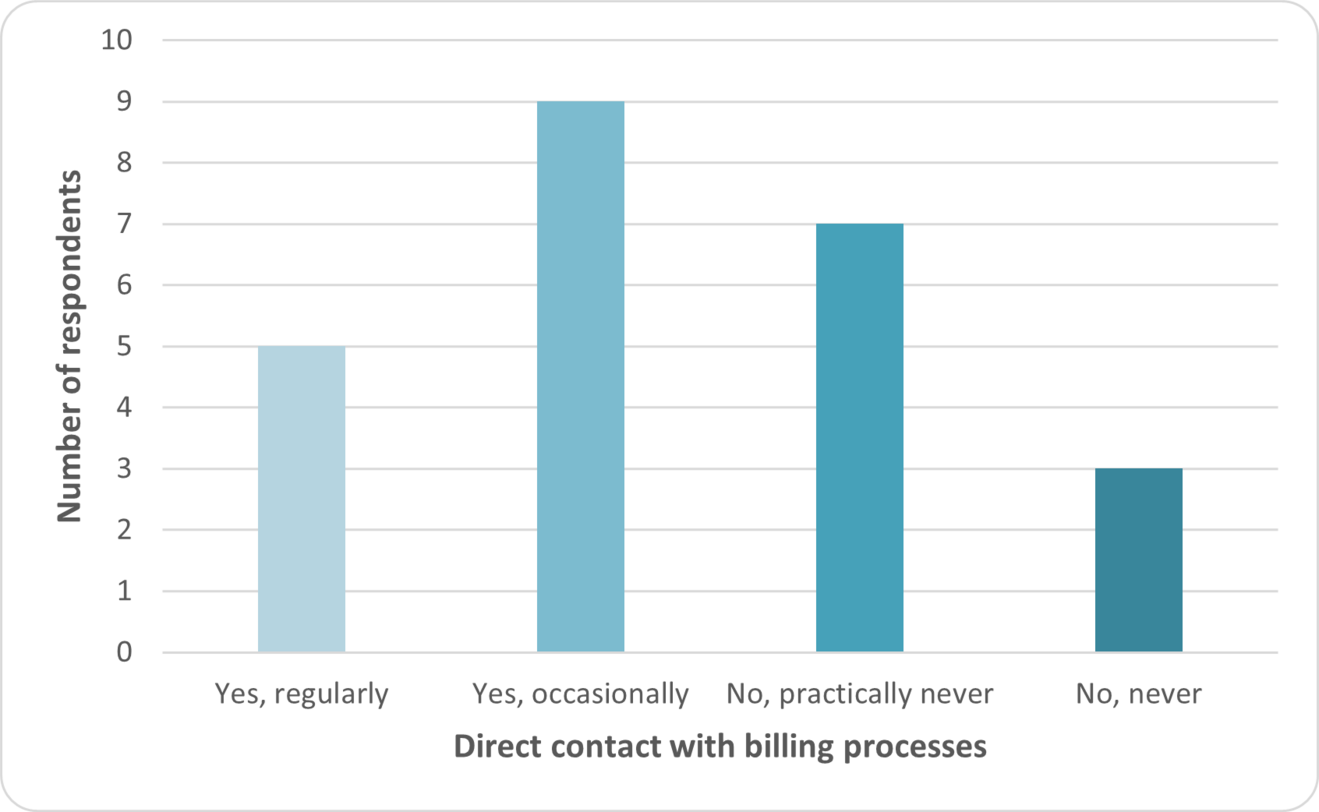
Direct involvement in billing processes was heterogeneous. Only 5/24 (21%) reported regular contact, whereas 10/24 (42%) reported little or no exposure.
Sources of information and barriers
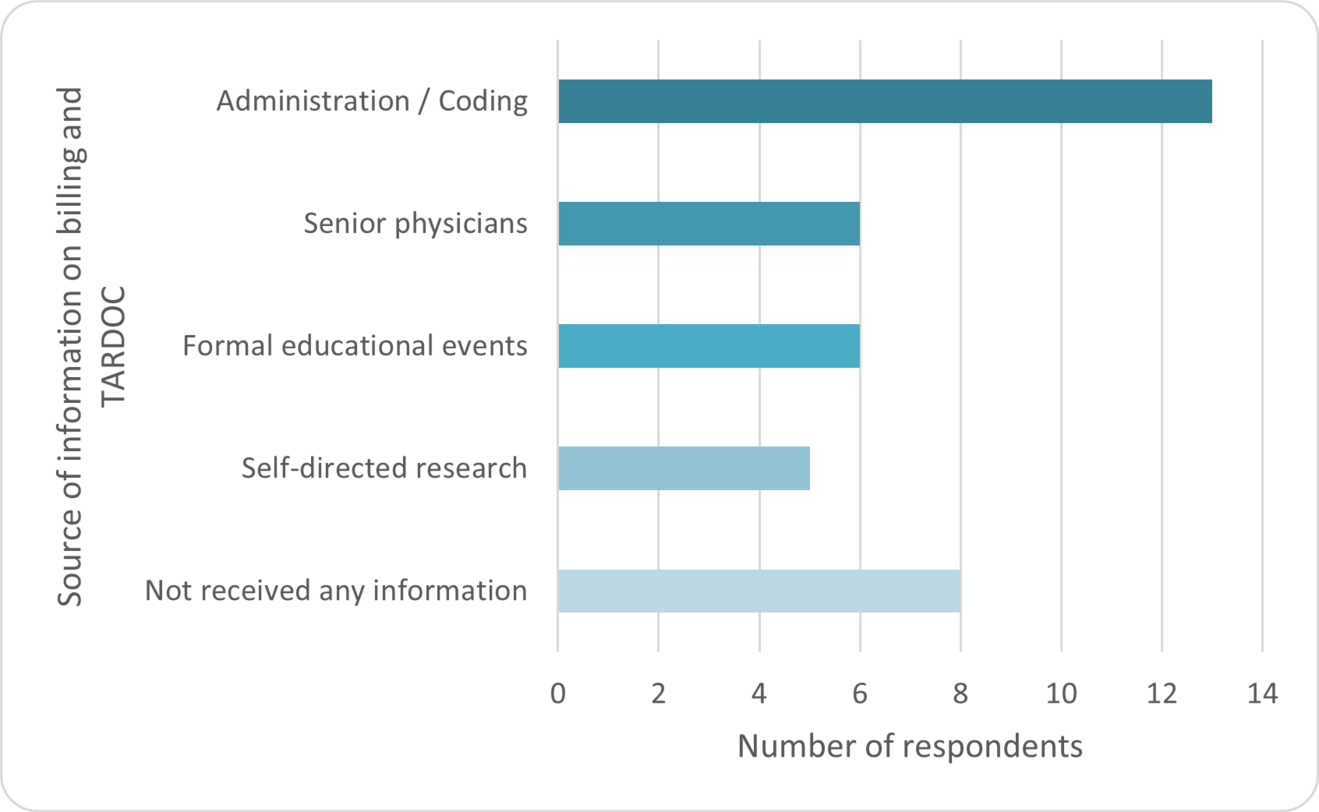
Information on billing and TARDOC was most frequently obtained through administrative or coding departments (13/24, 54%), while 8/24 (33%) reported having received no information at all.
The most common barriers to engagement were lack of time and prioritization of clinical duties (19/24, 79%), delegation of billing responsibilities (12/24, 50%), fixed salary structures (12/24, 50%), and lack of formal teaching (12/24, 50%). Moreover, 25% (6/24) of respondents perceived the topic to be irrelevant to the daily work and 20,83% (5/24) as to be too complex.
Perceived importance and training needs
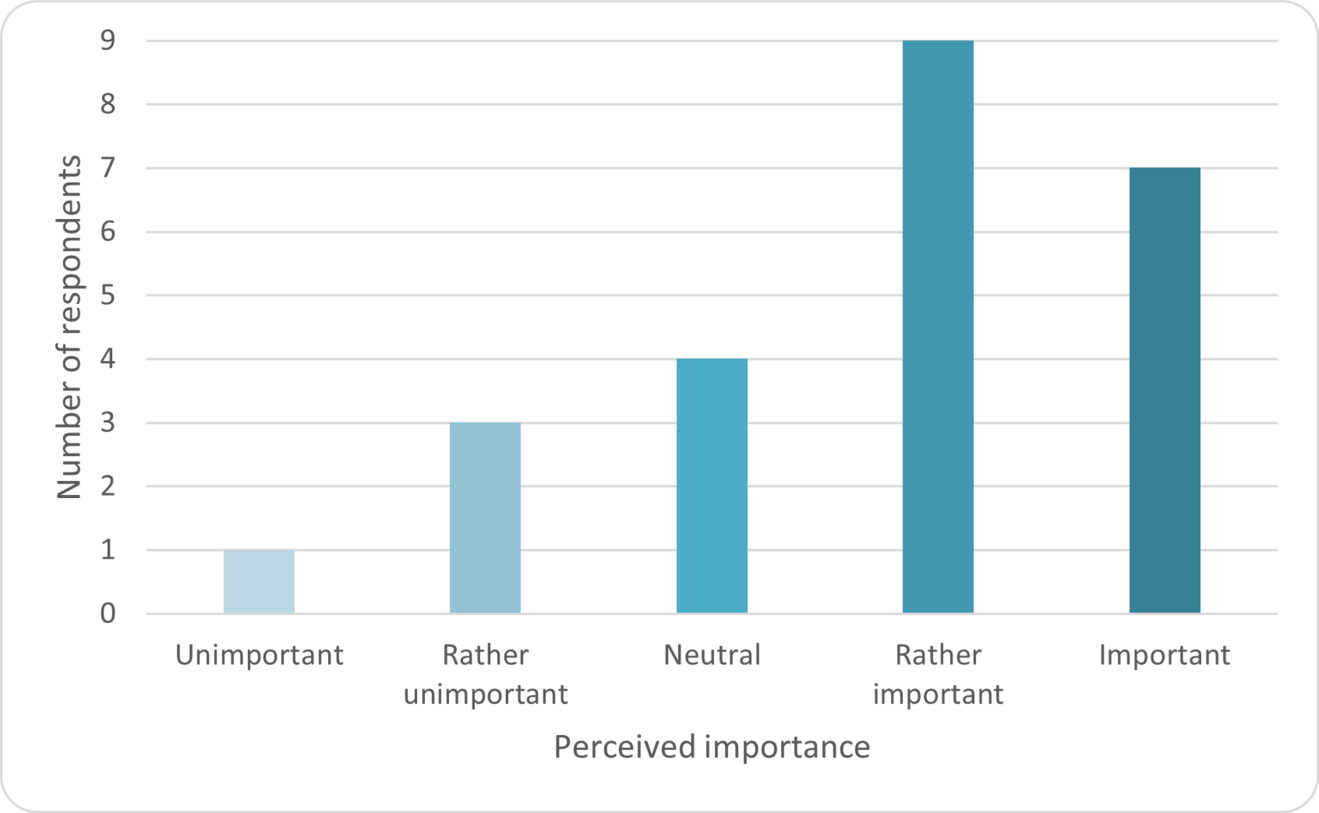
Despite limited familiarity, 16/24 (67%) considered billing knowledge important or rather important for residents, while only 4/24 (17%) considered it unimportant.
Half of respondents (12/24, 50%) had never received any formal training on billing or TARDOC. Nevertheless, 23/24 (96%) expressed interest in training, most preferring short or basic formats (15/24, 63%).
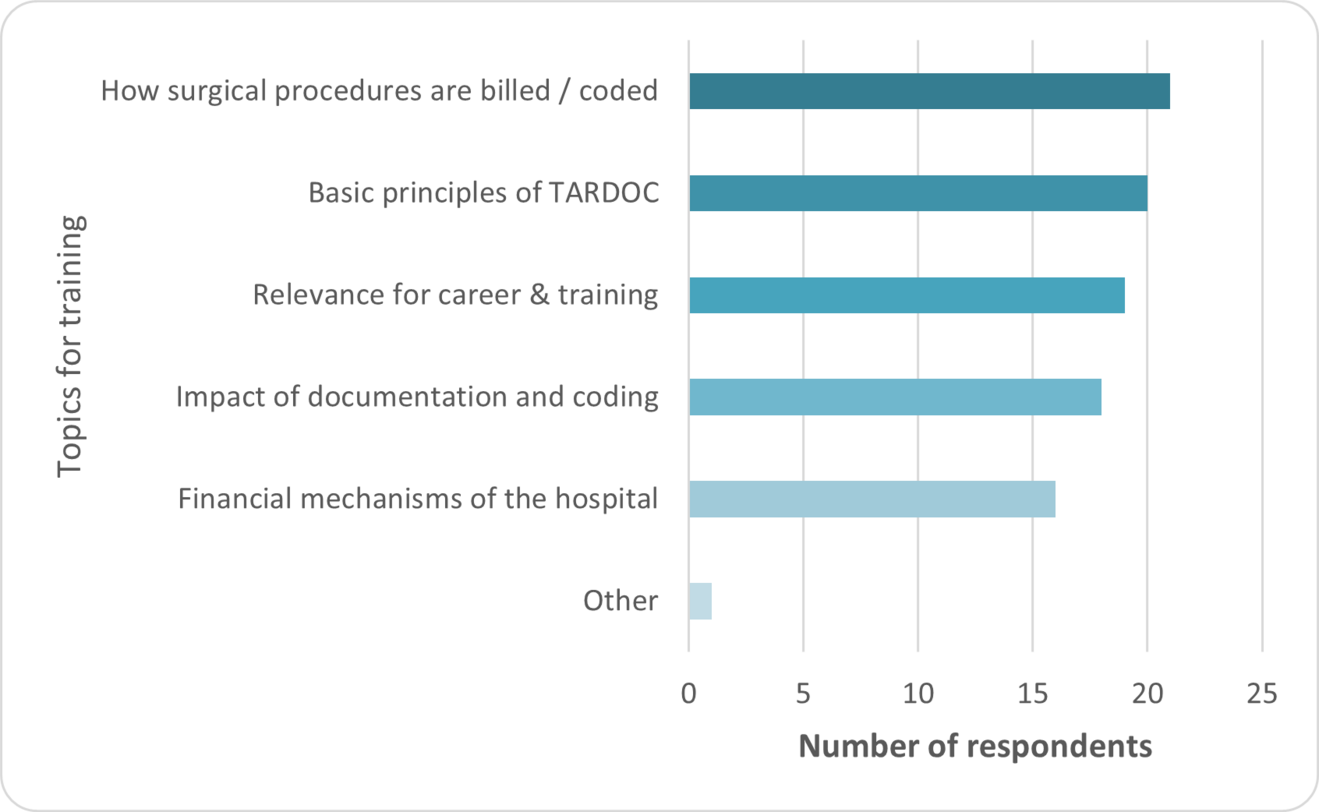
Desired topics focused on practical aspects, including how surgical procedures are billed (21/24, 88%), basic principles of TARDOC (20/24, 83%), and relevance for career development (19/24, 79%).
Work priorities and perceived indirect impact
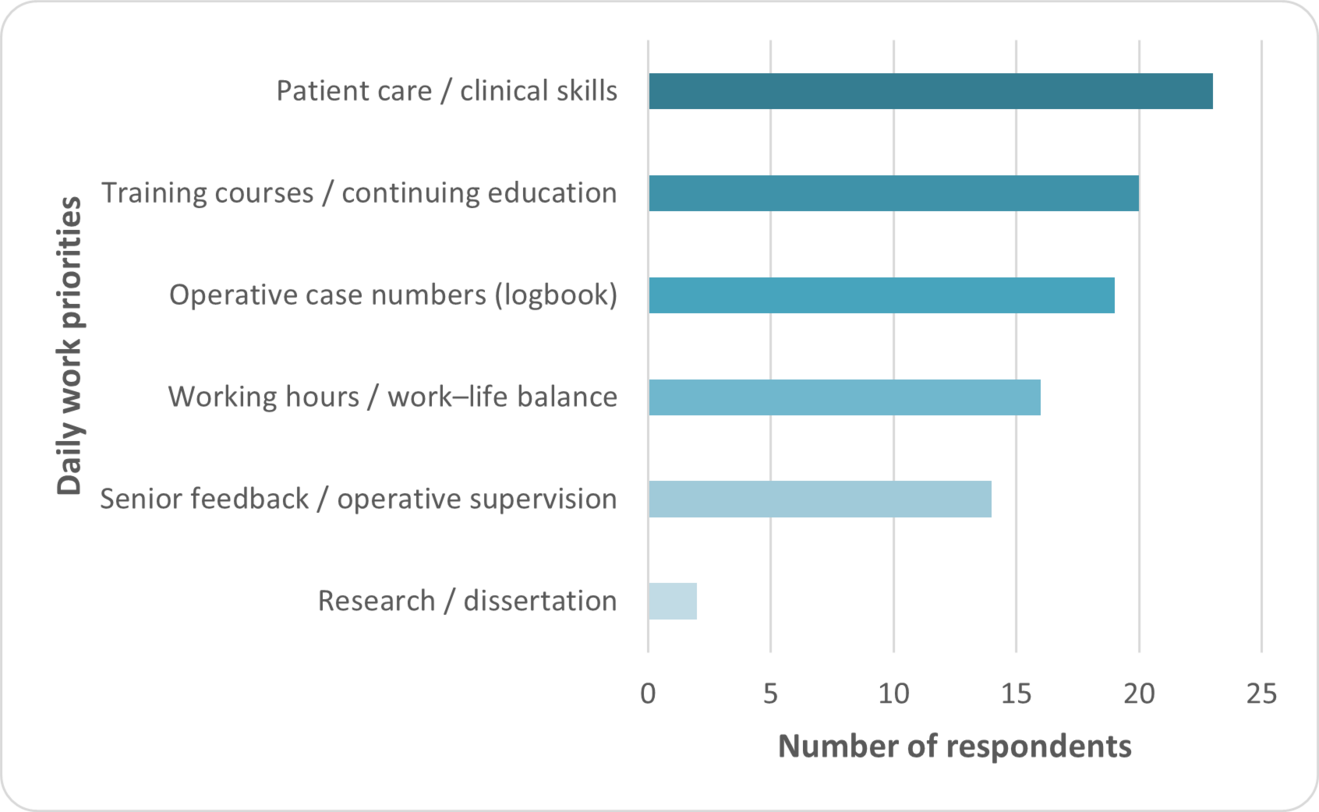
Clinical duties and training requirements clearly outweighed billing issues as daily priorities, particularly patient care (23/24, 96%) and operative training requirements (19/24, 79%).
Despite limited direct involvement, 16/24 (67%) perceived that billing-related issues indirectly influenced their daily work.
Qualitative insights
Open-ended responses emphasized that billing is a fundamental but insufficiently taught aspect of healthcare, with concerns about patient financial consequences and a perceived lack of institutional responsibility for education.
Discussion
This exploratory survey demonstrates a clear mismatch between the perceived importance of billing knowledge and the limited familiarity and exposure reported by Swiss surgical residents following the introduction of TARDOC. Importantly, this gap was observed despite a respondent cohort skewed toward senior trainees and large institutions—arguably a best-case scenario for billing exposure.
The predominance of structural barriers, such as time constraints and delegation of billing responsibilities, aligns with international findings showing that billing education is inconsistently integrated into postgraduate training [5–7]. Our results support the concept of a “hidden curriculum,” in which economic mechanisms shape clinical practice without being explicitly addressed in training. Integrating concise, practice-oriented billing education into surgical training programs may improve transparency and preparedness without competing with core clinical priorities.
Limitations
The small sample size and voluntary participation introduce selection bias, with overrepresentation of senior residents and large hospitals. Data are self-reported and descriptive, and no inferential analyses were performed. Results should therefore not be generalized beyond the exploratory context.
Conclusion
In the early phase of TARDOC implementation, surgical residents report limited billing literacy despite recognizing its relevance and expressing strong interest in structured education. Even among senior trainees, billing knowledge remains low, underscoring the need for institutionally supported, practice-oriented educational initiatives.
- Eonum AG. Tariffs in the Swiss healthcare sector.
- Federal Office of Public Health (FOPH). Outpatient medical tariff: TARDOC and outpatient flat rates.
- Walder Wyss Ltd. Federal Council approves new outpatient tariff system. 2025.
- DayOne Switzerland. Supporting Swiss hospitals in the transition to TARDOC and outpatient flat rates.
- Faux M, Adams J, Wardle J. Educational needs of medical practitioners about medical billing: a scoping review. Hum Resour Health. 2021;19:84.
- Austin RE, von Schroeder HP. Billing knowledge and exposure during residency training. BMC Med Educ. 2019.
- Paz KB et al. Medical coding and billing training in U.S. residency programs. J Drugs Dermatol. 2018;17:678–682.