The project is supported and funded by the Swiss Armed Forces’ Center for Military and Disaster Medicine (MKM), whose cooperation is gratefully acknowledged.
In modern warfare, the injury patterns of combat casualties are characterized by high-energy blast trauma, penetrating injuries frequently involving multiple organ systems, associated burns, traumatic amputations and severe hemorrhage. These injuries often occur in operational environments where rapid evacuation and early access to advanced medical facilities cannot be assumed.
In Switzerland and Central Europe, emergency and trauma care systems are highly optimized for civilian injury mechanisms, which are predominantly blunt and typically managed within short transport times to definitive care. Penetrating and blast-related injuries, massive hemorrhage, and traumatic amputations remain rare in routine clinical practice. Consequently, both civilian trauma teams and military medical units have limited opportunities to acquire practical experience in managing these injury patterns that characterize modern combat scenarios. This limited exposure may have significant implications for national preparedness should comparable injury mechanisms arise in military, civilian, or hybrid threat settings. In this article, we present initial findings from an ongoing multicenter, interdisciplinary and interprofessional, simulation-based initiative addressing a geopolitically urgent and highly relevant challenge.
Simulation-based training has become an essential tool for preparing healthcare professionals for rare but high-consequence events, while simultaneously improving technical skills and non-technical team performance factors. High-fidelity simulations using trained actors and advanced patient simulators allow complex clinical scenarios to be reproduced in a controlled, standardized, and psychologically safe environment. In the context of combat trauma, simulation also provides the opportunity to integrate surgical and anesthesiological skills with operational constraints, such as prolonged prehospital phases and limited resources.
We developed a collaborative initiative between the Swiss Armed Forces and several civilian trauma centers. The scenario is inspired by real-world combat injury patterns and is designed to reflect key clinical and operational characteristics of contemporary combat trauma care. The primary objective is to evaluate the quality and timeliness of critical interventions and to identify team performance patterns that may inform future training strategies and strengthen interdisciplinary collaboration. Civilian and military medical teams from different levels of care and professional backgrounds will participate, enabling evaluation under comparable and controlled simulation conditions. This approach is particularly relevant, as experience from recent conflicts has demonstrated that in the era of forward surgical teams, micro-hospitals, and high-mobility medical concepts, the boundaries between prehospital and in-hospital care are increasingly blurred.
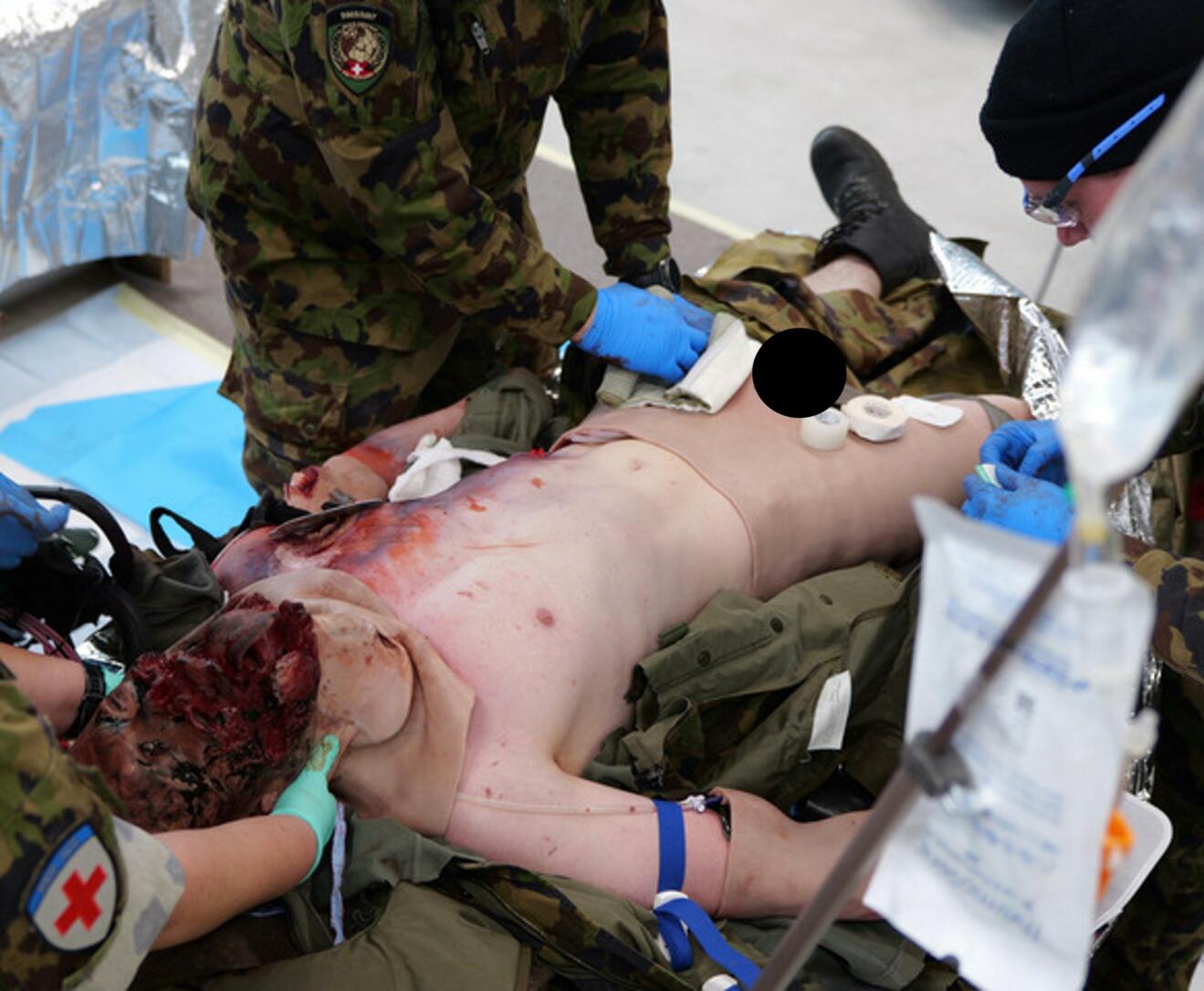
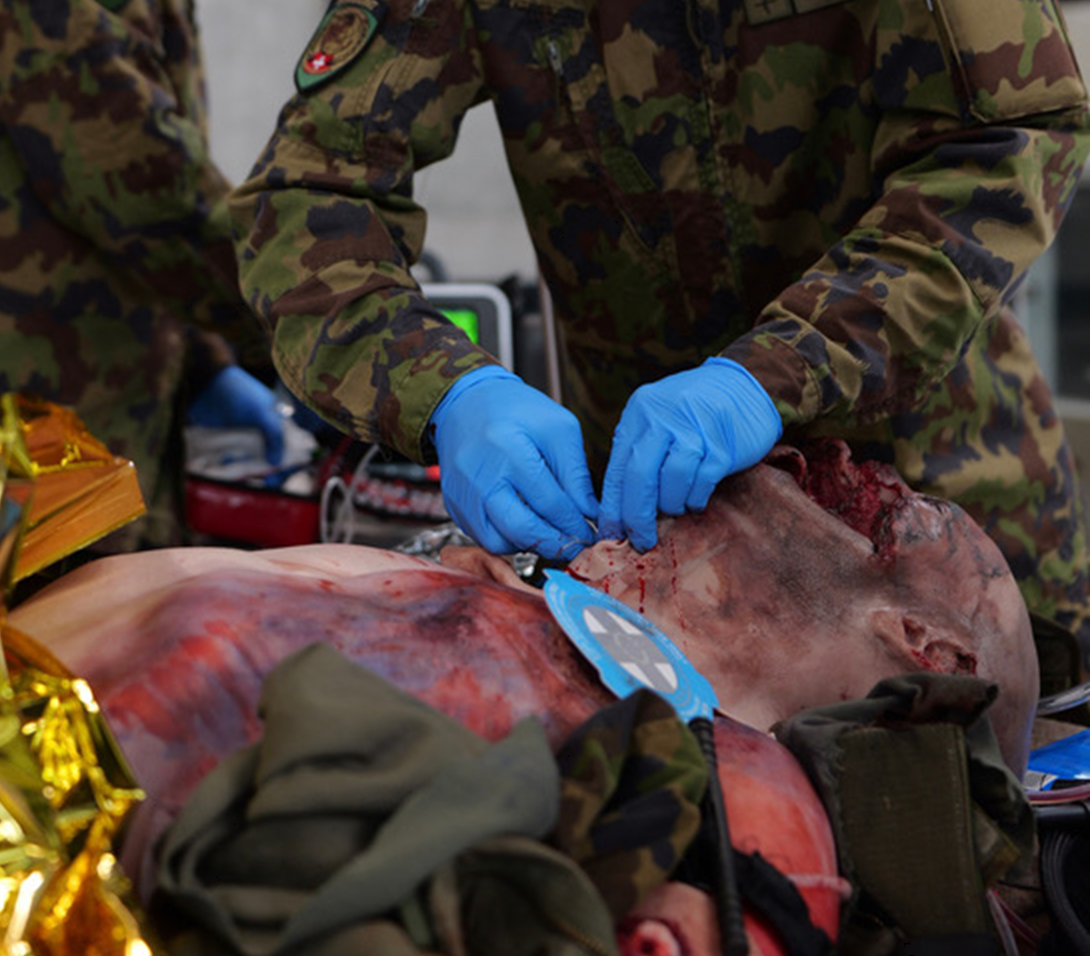
The simulation scenario is specifically based on a video recording from an active conflict zone documenting an improvised explosive device (IED) detonation. Injuries are represented using advanced moulage techniques and professional make-up and include severe maxillofacial trauma with progressive airway obstruction, multiple hemorrhage sites, an evolving tension hemothorax, and associated injuries such as burns and extensive soft-tissue trauma. Modern simulation equipment allows bleeding sites to be connected to pump systems delivering simulated blood and the majority of critical interventions – including surgical cricothyrotomy, intravenous and arterial access, and hemorrhage control – can be performed directly on the simulated patient. Thoracic interventions, such as needle decompression or finger thoracostomy, are performed on an external task trainer when required. Multiple Pilot simulations were conducted before study start at the Zurich Polytrauma Course at the University Hospital Zurich in September 2025 with a group of international trauma surgeons. Feedback from these pilot sessions was used to refine the simulation scenario, assessment tools and study procedures.
To date, we have conducted approximately 20 simulations with diverse civilian and military teams across various settings, ranging from in-hospital resuscitation bays to outdoor environments. Over the coming months, additional simulations will be performed at further centers, with the goal of completing a total of 30 fully evaluated scenarios. The simulations conducted thus far demonstrate substantial interest in the topic of combat-related injuries and in civil–military collaboration across all levels of trauma care. One preliminary observation is that hospital-based teams experienced greater difficulty achieving rapid hemorrhage control, particularly in identifying exit wounds in patients with multiple shrapnel injuries. A possible explanation is that the clinical “X” component (exsanguinating hemorrhage control) was only formally incorporated into the ATLS primary survey algorithm in 2023, whereas in prehospital and military settings, immediate bleeding control has long been embedded in structured approaches such as XABCDE and MARCH. However, across all participating groups, we observed delays in the timely identification and control of major external bleeding on both the anterior and posterior body surfaces. Additional differences were noted in the choice of thoracic decompression techniques (needle decompression versus finger thoracostomy), as well as in the timing and strategy of blood product administration and pharmacologic coagulation optimization.
In military contexts—strongly influenced by U.S. doctrine—early fluid resuscitation with packed red blood cells or whole blood plays a central role and is firmly integrated into Tactical Combat Casualty Care (TCCC) guidelines, whereas crystalloid fluids are no longer recommended. In contrast, current European major bleeding guidelines continue to include crystalloids with a 1B level recommendation, reflecting ongoing differences in practice paradigms. We look forward to completing the remaining simulations and conducting a comprehensive analysis of the results. Our objective is to generate actionable insights to enhance preparedness and optimize the management of complex combat-related injury patterns within the Swiss trauma system. Furthermore, by publishing our detailed study protocol, simulation scenarios, and structured assessment framework, we aim to facilitate national and international collaboration and encourage other research groups to implement similar initiatives.